
Not quite menopause. Throwing blankets off at night, keeping awake. Fatigue and irritation punctuated throughout the day by heat dissipating from every pore, clouding thoughts, reinforcing forgetfulness. Hair falling out so stubbornly fast. Clothes choosing when to fit. Flooding periods coming sporadically, unexpectedly. They call it “the change of life” – but I feel like a different person altogether. What is happening?
In perimenopause, the physiological landscape is subject to tremendous change with estradiol and progesterone at the heart of the transition. Progesterone levels fall quickly – no ovulation – no corpus luteum – no progesterone. Estradiol, on the other hand, does not give up so easily. Estradiol levels continue to rise and fall – reliable, steady, wave-like – a biological rollercoaster – approaching the halting rhythms of reproductive senescence. In the context of very low progesterone, these dramatic peaks and troughs in estradiol levels, give rise to systemic consequences and unrelenting symptoms of the menopausal transition.
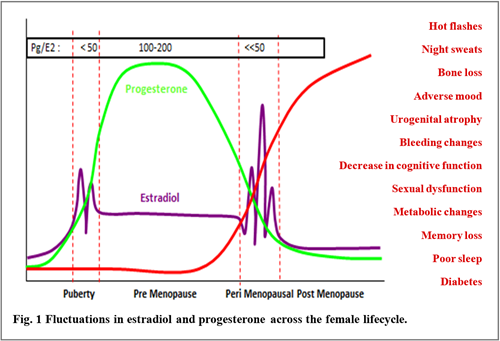
Hot flashes, synonymous with menopause, commonly co-occur with other neurological symptoms – mood changes, sleep disturbances and decline in cognitive function [1]. Many of these are naturally attributed to the shifting hormonal milieu. Although historically ascribed to strictly reproductive functions, hormones serve as important neural substrates. For example, adequate estradiol levels are essential to neuronal health with its neuroprotective and antioxidant properties [2]. As estradiol levels plummet in menopause, neurological dysfunction arises from the impaired glucose homeostasis, mitochondrial dysregulation, and attenuated ATP production.
Estradiol and Serotonin
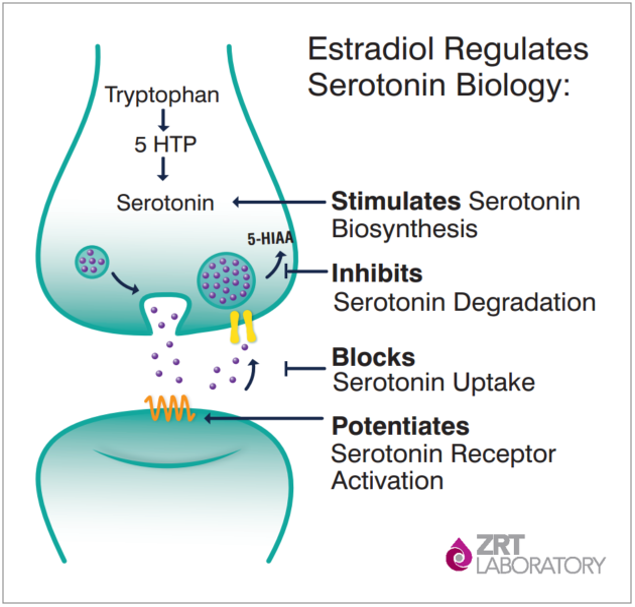 Fig. 2. The importance of estradiol in modulating serotoninergic tone.
Fig. 2. The importance of estradiol in modulating serotoninergic tone.Specific to neurotransmitter systems, estradiol has a close-knit relationship with serotonin, aptly nicknamed "the happiness molecule." Estradiol directly modulates just about everything about serotonin biology:
- Upregulates the expression of tryptophan hydroxylase, the enzyme in charge of the rate-limiting step in the serotonin biosynthesis pathway;
- Helps augment serotonin receptor activation and subtype expression;
- Blocks re-uptake; slows down degradation by suppressing monoamine oxidase expression – the enzyme that rapidly breaks down serotonin into inactive form. In other words, in order to have enough serotonin around, you need adequate estradiol levels.
So What Happens in Menopause?
When the maestro steps off the podium, despite years of exquisite discipline and arduous practice, the permanence of the loss drives the symphony to disarray. As estradiol firmly sets a course to wind down (albeit not without a fight), the serotonin system experiences this deficiency first-hand. With little estradiol left to stimulate tryptophan hydroxylase expression, this translates to reduced intrinsic serotonin production. Serotonin production is further reduced by increased monoamine oxidase expression (no more estradiol to keep suppressing its overexpression) – rapidly metabolizing what little serotonin there is to begin with.
The newly acquired low serotonin tone perpetuates the tenacity of unremitting sleepless nights, hot flashes, mood swings, and brain fog. This is why some women can be helped with SSRI therapy – blocking the reuptake of what's left of serotonin to help take the edge off the severity of hot flashes or mood swings [3] [4]. However, SSRI therapy comes with a slew of its own side effects especially lowered libido (also worsened by low estrogen) and GI side effects. Plus, without estradiol in the picture, all the other symptoms of menopause – bone loss, vaginal dryness, glucose dysregulation, metabolic changes, cardiovascular health – remain unaddressed.
A Common Picture in Perimenopause
Below is an example of a laboratory work-up for a perimenopausal patient presenting with a clinical picture of symptoms and results, commonly observed at ZRT. Weight gain, sleep disturbances, fatigue, and decreased libido can be explained in part by the low levels of estradiol and progesterone despite normal levels of testosterone.
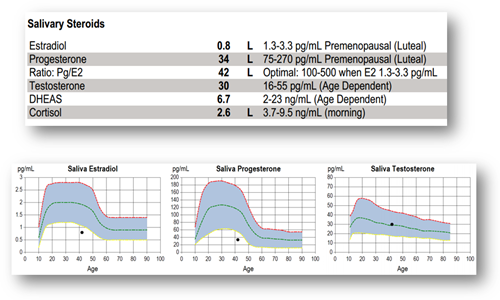
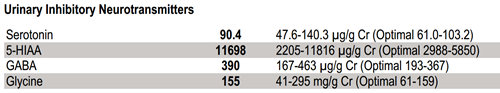
Low estradiol plays a role in steering neurotransmitter levels. Although this patient's serotonin levels are normal (she is not in menopause yet), the levels of the serotonin metabolite, 5-HIAA are above the optimal range, suggesting that she is starting down the path of increased serotonin metabolism. There is a discordance in the results – serotonin, the precursor is lower in the clinical range than 5-HIAA, the metabolite. Without intervention, as time goes by, the gap between the two may widen – as estradiol levels continue to decline, further accentuating existing symptoms and allowing for new symptoms to develop.
Keeping an eye on emerging hot flashes, night sweats and changes in bleeding patterns is important when looking for imminent signs of menopause. Low progesterone and fluctuating estradiol as part of the normal physiological change are expected during the transition and can be picked up by a non-invasive saliva test. Low estradiol, driving serotonin and 5HIAA into discordant clinical ranges, is also typical and can be observed with urinary neurotransmitter analysis.
What's a Woman to Do?
As perimenopausal signs emerge, working with a practitioner who uses low-dose, bio-identical hormone replacement therapy judiciously to alleviate symptoms and rectify hormonal balance is crucial to maintaining mood and reducing debilitating symptoms. Of course, regular hormone testing to ensure levels remain in physiological ranges is important. Nurturing mental health during this time of transition is not only a matter of addressing hormonal balance; women also benefit from the support and understanding of their loved ones as they begin to behave in uncharacteristic ways, and from taking time to care for themselves and acknowledging their bodies’ altered needs.
Related Resources
- Blog: Menopause - Is it All in Your Head?
- Blog: Estrogen: The Link Between Microbiome, Menopause & Metabolic Health
References
[1] Brinton, R.D., et al., Perimenopause as a neurological transition state. Nat. Rev. Endocrinol, 7/2015. 11(7): p. 393-405.
[2] Fischer, B., C. Gleason, and S. Asthana, Effects of hormone therapy on cognition and mood. Fertil. Steril, 4/2014. 101(4): p. 898-904.
[3] Freedman, R.R., Menopausal hot flashes: mechanisms, endocrinology, treatment. J Steroid Biochem. Mol. Biol, 7/2014. 142: p. 115-120.
[4] Krause, M.S. and S.T. Nakajima, Hormonal and nonhormonal treatment of vasomotor symptoms. Obstet. Gynecol. Clin. North Am, 3/2015. 42(1): p. 163-179.
